A model of cancer screening
The mathematics also permitted the development of a computer simulation model of cancer growth, spread, and detection, which could determine the impact of various usages of screening, and especially of various screening intervals, on the reduction in death achievable by screening.
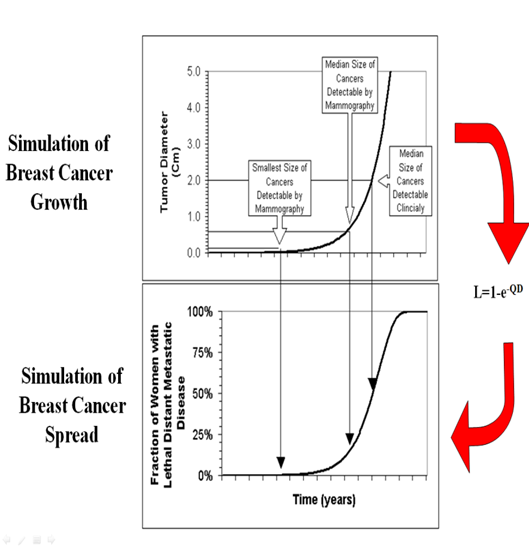
While randomized trials have shown that mammographic screening saves lives, critical questions concerns the optimal age of screening initiation and screening interval. A computer simulation model of breast cancer growth, spread, and detection, which could calculate the reductions in death, and costs, resulting from various screening intervals and ages of screening initiation. The simulation revealed that breast cancer survival of 90+% appears to be achievable, if women are screened annually. The ACS recommendation of yearly screening from age 40 appears to be a highly effective strategy, yielding a population-wide breast cancer survival of 88%, which corresponds to a 66% population-wide reduction in death. Less intensive screening strategies, such as screening every second or third year, not screening until age 50, or ending screening at 70, should yield markedly worse outcomes, while the pattern of screening used in the United Kingdom of every 36 months from age 50 to 70 is very ineffective, achieving only a 12% reduction in death. There appears to be no upper age limit for screening. A small additional reduction in the breast cancer death rate appears to be achievable by decreasing the screening interval to every six months, and by decreasing the age of screening initiation to age 30, but there appears to be little additional benefit from going beyond this. Prompt annual mammographic screening from age 40 appears to be capable of leading to considerable reductions in breast cancer lethality, with a small additional benefit to be derived from screening as frequently as twice a year from age 30.